Knee pain affects approximately 25% of adults. Initial management typically includes physical therapy, oral or topical NSAIDs, and corticosteroid injections, but these measures provide only partial relief, leaving many patients with pain or functional limitations after months of standard care. As a result, clinicians are turning to evidence-based regenerative treatment for knees to promote tissue healing rather than masking symptoms.
Why Conservative Knee Treatments Often Fail
Conservative care can reduce pain and improve function, yet effect sizes are modest and transient for many patients. Meta-analytic data show NSAIDs provide short-term relief with benefits that diminish as treatment continues and a known risk profile for adverse events (Thomsen et al., 2021). Repeated intra-articular corticosteroid injections may further complicate the picture, with randomized data showing greater cartilage volume loss over two years and no superior pain relief versus saline in knee osteoarthritis (McAlindon et al., 2017).
Even with structured nonoperative programs, a subset of patients does not reach durable clinical improvement and later proceeds to surgery. Trials comparing surgical and nonsurgical pathways in knee osteoarthritis demonstrate that total knee replacement yields larger gains in carefully selected candidates, underlining the limits of conservative modalities in advanced disease (Skou et al., 2018). When pain persists or function declines despite therapy, analgesics, or injections, a regenerative treatment for the knees becomes a reasonable next step before definitive arthroplasty.
Regenerative Therapies for Knees After Failed Conservative Care
When conservative care no longer provides relief, clinicians often turn to regenerative treatment to stimulate healing at the tissue level. These therapies are designed to enhance intrinsic repair processes by encouraging cartilage preservation, tendon recovery, and restoration of subchondral bone rather than simply masking pain. Unlike medications or injections that primarily suppress inflammation for short-term benefit, regenerative approaches actively drive biologic repair, improve blood flow, and modulate the inflammatory response toward balance, improving pain and function in knee conditions.
Candidates are typically patients with persistent knee pain or limited function despite conservative care, who wish to delay surgery but still require meaningful improvement. Let’s explore how some of the most widely used regenerative treatments in clinical practice apply these principles to knee care.
SoftWave Therapy
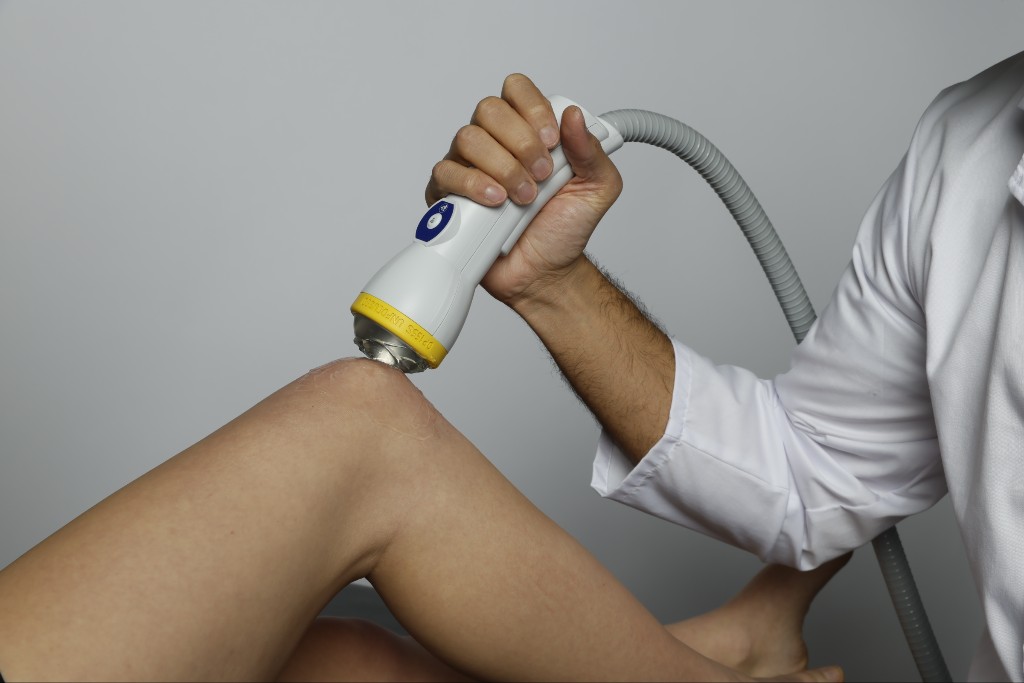
SoftWave Therapy offers a broad-focused shockwave solution designed to stimulate regenerative healing in the knee joint. Its patented parabolic reflector shapes parallel shock waves that penetrate up to 7 cm deep and 12 cm wide, covering both superficial and deep tissues in a single session without creating microtrauma. With FDA 510(k) clearances for activation of connective tissue, increased local blood circulation, and relief of minor aches and pains, along with additional wound and burn indications, it provides a safe and practical outpatient option for musculoskeletal care.
Clinical evidence supports its regenerative impact. In patients with knee osteoarthritis, a randomized controlled trial of extracorporeal shockwave therapy showed significantly greater improvements in pain and function compared with sham treatment after just four weeks (Zhong et al., 2019). Protocols are efficient, typically lasting about ten minutes, require no anesthesia, and can be standardized for consistent use across clinical practices. This makes SoftWave Therapy a leading non-invasive option for clinicians expanding regenerative treatment for knees.
Learn more about the Best Shockwave Therapy Machine for Providers.
Platelet-Rich Plasma (PRP)
PRP is an autologous preparation in which platelets are concentrated from the patient’s own blood and injected into the joint, delivering growth factors such as PDGF, TGF-β, and VEGF. In knee osteoarthritis, proposed effects include modulation of synovial inflammation, support of chondrocyte activity, and influence on subchondral bone health. Randomized trials have reported that PRP can improve pain and function compared with hyaluronic acid, though variability in preparation methods and patient response makes outcomes inconsistent across studies (Tang et al., 2020). Standardization of protocols and careful patient selection remain important considerations for its use in clinical practice.
Micro-Fragmented Adipose Tissue (MFAT)
MFAT is prepared from mechanically processed lipoaspirate, preserving stromal vascular fraction and extracellular matrix elements that act through paracrine to influence inflammation, cartilage activity, and subchondral remodeling. It is typically considered for patients with symptomatic osteoarthritis who have not improved with other conservative approaches. Evidence from a prospective case series reported that patients receiving MFAT experienced improvements in WOMAC and KOOS scores over follow-up, though responses varied and the findings were observational in nature (Russo et al., 2023).
Bone Marrow Aspirate Concentrate (BMAC)
BMAC is an autologous concentrate derived from bone marrow that contains mesenchymal stromal cells, hematopoietic cells, and cytokines. It is used in some patients with knee osteoarthritis as an option after conservative treatments have not provided sufficient relief. A randomized trial comparing BMAC with hyaluronic acid found similar outcomes for pain and function over a two-year period, indicating that while BMAC may provide benefit, it has not consistently demonstrated superiority to other injectable therapies (Boffa et al., 2022). Standardization of harvesting techniques and appropriate patient selection remain important considerations in its clinical use.
Expand Your Treatment Capabilities With SoftWave Therapy
When conservative measures to knee conditions fall short, regenerative approaches provide a way to target underlying joint biology. Treatments such as SoftWave Therapy and orthobiologics have demonstrated the potential to modulate pain and improve function in knee degenerative conditions, offering clinicians additional tools beyond symptom control.
SoftWave Therapy devices build on this evidence with technology designed for broad tissue coverage, efficiency, and integration into diverse specialties, including orthopedics, sports medicine, physical therapy, urology, and podiatry. Further clinical insights are available through SoftWave TRT’s research library, supporting informed application in practice.
Become a Provider or Schedule a Demo today to bring SoftWave to your clinical program.