Shockwave therapy has expanded across musculoskeletal and regenerative care, yet devices differ meaningfully in energy generation, treatment field geometry, and how consistently the dose can be delivered across patients and operators. DolorClast Therapy is commonly positioned within this landscape, most often in radial and focused protocols for musculoskeletal pain presentations. While published studies do reference the radial DolorClast in selected indications, the evidence base is concentrated in specific conditions and frequently emphasizes symptom outcomes over independent validation of treatment zone size, depth distribution, or tissue volume engagement.
For clinicians, understanding what is supported in device-named literature and what still relies on extrapolation from broader radial shockwave research helps set appropriate expectations for protocol design and reproducibility in practice.
What DolorClast Therapy Claims To Be
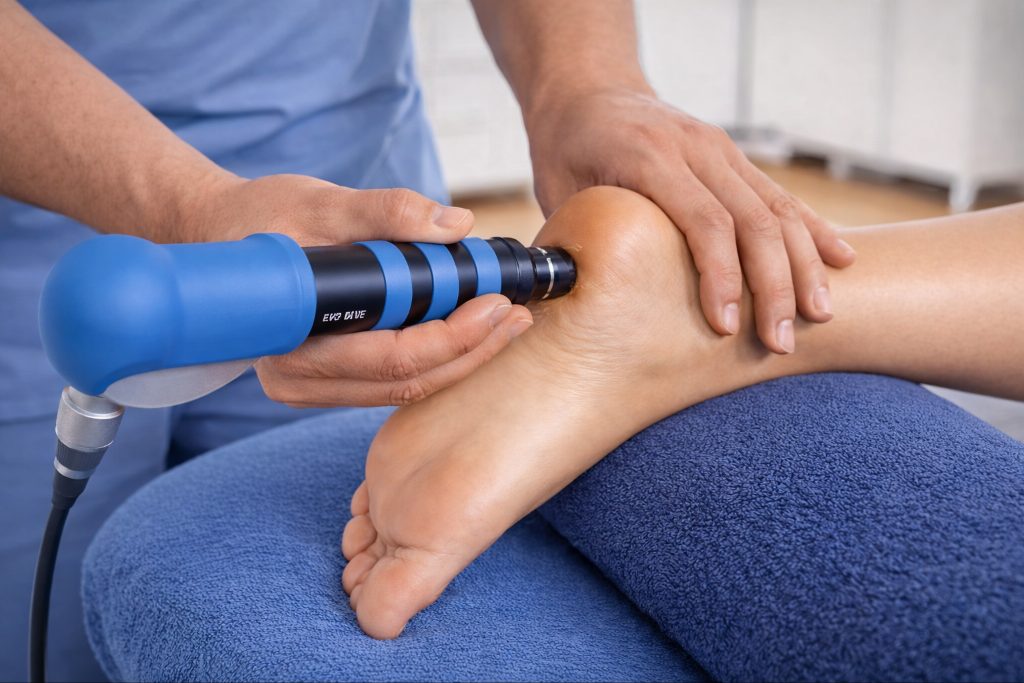
DolorClast systems are presented as extracorporeal shockwave platforms that include radial and focused configurations. In manufacturer descriptions, the radial system uses pneumatic energy generation to deliver a dispersing pressure wave from the applicator into superficial soft tissue. The focused configuration is positioned for deeper, more localized targeting where energy is concentrated along a defined path.
In manufacturer positioning, DolorClast is commonly associated with plantar fasciopathy, tendinopathies, and shoulder pain syndromes. In device-named literature, DolorClast is referenced most often in radial protocols studied in defined musculoskeletal cohorts, including knee osteoarthritis and adhesive capsulitis.
Only a few points about DolorClast can be stated with confidence:
- Device-named trials most often evaluate radial DolorClast protocols in discrete musculoskeletal presentations such as knee osteoarthritis and adhesive capsulitis. Imamura et al. (2017), Zhang et al. (2021). Hussein et al. (2018).
- Reported outcomes commonly rely on pain and function instruments such as VAS and WOMAC, with less frequent reporting of objective tissue-level or imaging endpoints in these device-named trials.
- Follow-up timelines are commonly short-term, which supports interpretation of near-term change while leaving longer-term durability less consistently addressed across cohorts.
- Technical reporting in device-named trials less often includes independent mapping of field size, depth profile, or tissue volume exposed, which can make protocol translation across anatomical regions less direct.
- In published musculoskeletal studies that name DolorClast, radial protocols are more common than focused protocols, so expectations for focused performance are often inferred from broader focused ESWT literature rather than from DolorClast-focused trials.
These publications help clarify where DolorClast has been studied directly in musculoskeletal care, while highlighting areas where technical characterization and device-named focused evidence are less developed in the published record.
Where Radial and Focused Shockwave Have Evidence in the Literature
Radial and focused shockwaves have been evaluated across multiple musculoskeletal populations, although outcomes vary across protocols, dosing strategies, and clinical endpoints.
These effects have been described in peer-reviewed studies:
- Plantar fasciopathy trial comparing radial ESWT, sham rESWT, or exercise added to advice and custom orthoses, with no added improvement over advice plus orthoses alone. Heide et al. (2024)
- Chronic plantar fasciitis randomized trial where device appearance did not influence radial ESWT outcomes, using patient-reported outcomes and ultrasound measures. Morral et al. (2019)
- Chronic plantar fasciopathy trial comparing recommended dose radial ESWT with minimal dose, reporting within-group improvement without between-group difference. Wheeler et al. (2022)
- Lateral epicondylitis randomized trial comparing focused shockwave with ultrasound therapy, reporting changes in pain and function outcomes. Król et al. (2024)
- Greater trochanteric pain syndrome randomized trial comparing focused shockwave therapy with ultrasound-guided corticosteroid injection using pain and function measures. Heaver et al. (2021)
- Bone stress injury runner series describing return-to-run outcomes after focused shockwave use in a clinical setting. Beling et al. (2023)
These findings reflect the broader radial and focused shockwave literature. They do not confirm device-specific output or treatment field geometry unless a named system is independently characterized. Operational and study design constraints that can limit protocol transfer across clinics and anatomical regions include:
- Results can shift with energy settings, pulse counts, session cadence, imaging guidance, and concurrent rehabilitation, even within the same diagnosis.
- Many papers report dose variables while providing limited detail on field geometry or the tissue volume exposed, which can make cross-region protocol translation less direct
- Endpoints are commonly centered on pain and function instruments, with fewer objective tissue-level endpoints or imaging-based biological correlates.
- Follow-up windows are frequently short to mid-term, which supports near-term interpretation while leaving durability less consistently characterized.
Read: Radial or Focused Shockwave Therapy? When to Use Each in Clinical Practice
DolorClast Therapy in Clinical Context and What Is Missing
Device-named DolorClast publications can inform selected radial musculoskeletal protocols, yet several evidence and reporting gaps remain when clinicians are building repeatable regenerative pathways across varied anatomy and symptom patterns.
Key areas to weigh in device evaluation include:
1. Limited Indication Breadth in Device-Named Studies
Named DolorClast studies tend to cluster in a small set of musculoskeletal cohorts rather than spanning the full range of tendinopathies and regional pain syndromes referenced in commercial positioning.
2. Outcome Focus That Is Mainly Symptom Based
Many reports rely on pain and function scales, with less frequent inclusion of objective tissue-level endpoints or imaging-based correlates.
3. Limited Independent Characterization of Field Geometry and Tissue Volume Engagement
Protocol variables such as impulses, frequency, and energy settings are often reported, while independent mapping of field size, depth distribution, and tissue volume exposure is less consistently documented.
4. More Device Named Evidence for Radial Than Focused Configurations
Within musculoskeletal publications that name DolorClast, radial protocols appear more frequently than focused protocols, which leaves focused expectations more dependent on broader focused ESWT literature.
These gaps do not negate the outcomes reported in the studied cohorts. They mainly shape how confidently protocols translate across regions, how reproducible dosing is likely to be in multifocal presentations, and how much additional technical validation a clinic may want when selecting a platform.
Why Broad Focused Shockwave Design Matters for Regenerative Indications
Many pain and function complaints are not driven from a single pinpoint lesion. Tendons, fasciae, muscles, periosteum, and perineural interfaces can all contribute, especially in chronic presentations where movement patterns and load tolerance have changed.
Broad-focused shockwave design is intended to address that layered reality through a larger therapeutic field. Rather than concentrating energy into a small focal point or dispersing it primarily near the applicator surface, a broad focused field is engineered to engage a wider tissue environment during each application. Clinicians often value this approach for regional tissue coverage and more consistent application across complex anatomy.
Clinical relevance that clinicians often consider:
- Coverage of superficial and deeper tissue layers within the same session
- Reduced dependence on exact handpiece placement when symptoms are multifactorial
- More consistent exposure across a region, which can support reproducibility across providers
- Practical efficiency for larger anatomical regions such as the shoulder girdle, hip complex, lumbar adjacent soft tissue, and posterior chain
- Patient tolerance considerations when protocols require higher total energy delivery over broader regions
SoftWave Therapy as a Broad Focused Shockwave Platform for Multispecialty Care
SoftWave Therapy is a patented, broad-focused shockwave platform intended for in-office clinical care. It uses an electrohydraulic source paired with a patented parabolic reflector to deliver a broad therapeutic field measuring roughly 7 cm by 12 cm. This design supports regional coverage that can reach superficial and deeper tissue layers during the same application.
SoftWave’s field architecture is used in protocols that aim to influence cellular activity associated with tissue repair, including inflammatory signaling, connective tissue activation, and neovascular responses. The delivery approach emphasizes distributed exposure across a larger zone rather than concentrating energy into a single focal point, which aligns with consistent patient tolerance across sessions.
SoftWave holds FDA 510(k) clearances that include activation of connective tissue, temporary increase in blood flow, temporary pain relief, treatment of chronic diabetic foot ulcers, and treatment of acute second-degree burns. The system is designed exclusively for clinical settings and is used across service lines, including orthopedics, podiatry, sports medicine, physical therapy, urology, and wound care.
For clinicians comparing architectures, the difference often comes down to treatment coverage. Radial systems typically disperse energy outward from the applicator with higher intensity near the surface, focused systems concentrate energy into a smaller target zone, and SoftWave delivers a broad field that supports engagement of a wider tissue environment within a single session.
How Clinicians Compare Shockwave Devices When Selecting a Platform
Clinicians evaluating shockwave systems often compare design and evidence characteristics that influence real-world reproducibility and workflow fit.
Key criteria commonly considered include:
- Therapeutic field size and shape relative to target anatomy
- Depth profile and whether a single application can engage superficial and deeper tissues
- Patient tolerance at clinically meaningful dosing
- Regulatory status and clearance language that aligns with the clinic’s service lines
- The quality of the device-named evidence in the indications the practice treats most often
- Consistency of output and how dosing is documented and repeated across sessions
- Operator dependence, including how sensitive outcomes are to exact targeting
- Practical workflow factors such as treatment time per region, session cadence, and throughput
- Serviceability and long-term reliability expectations for high-volume clinical use
Selecting the Right Shockwave Platform for Clinical Practice
DolorClast sits within the broader shockwave landscape as a system family that includes radial and focused configurations, with published device-named musculoskeletal evidence more commonly tied to radial protocols. That literature can inform selected use cases, while leaving open questions that matter for broader protocol development, such as how consistently treatment field characteristics translate across anatomical regions and service lines.
Broad-focused shockwave systems, such as SoftWave, are designed to engage larger tissue volumes in a single application and hold FDA 510(k) clearances across indications relevant to connective tissue activation and temporary pain relief. When selecting a platform, clinicians often weigh regulatory alignment, evidence quality, treatment field design, patient tolerance, and workflow efficiency to ensure the system fits their patient population and clinic structure.
Learn more about the best Shockwave Therapy machine for providers.
Explore How SoftWave Fits Your Clinic Workflow
SoftWave is a patented, broad-focused shockwave system built for in-office care, with FDA 510(k) clearances that support use across connective tissue activation and wound-related indications alongside temporary blood flow and pain effects.
Clinicians who want to understand how SoftWave protocols translate into day-to-day practice can review published clinical data, consider specialty-specific use patterns, or evaluate workflow through a guided demonstration.
Learn more about SoftWave clinical research.