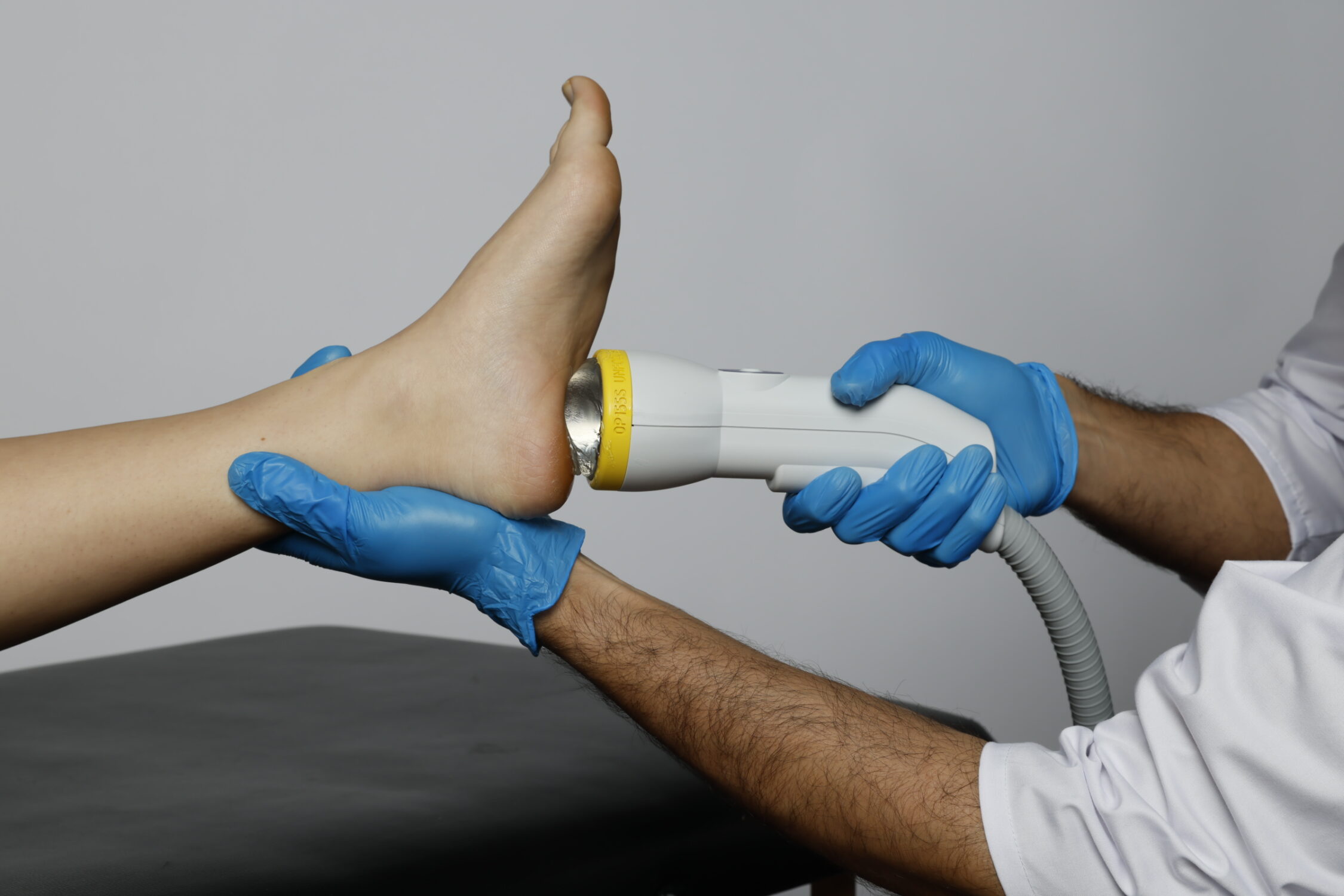
Shockwave therapy is increasingly recognized as a non-invasive option for a variety of conditions. It works through acoustic pulses that interact with tissue, producing both mechanical and biological effects that can support healing and reduce pain. Within this therapy, treatments are generally classified by the energy applied. Low-intensity shockwave therapy (LiSWT) and high-intensity shockwave therapy (HiSWT) represent two distinct approaches, each with unique characteristics and clinical considerations.
What Is High-Intensity and Low-Intensity Shockwave Therapy?
Low-intensity shockwave therapy uses energy levels below 0.2 mJ/mm². At these settings, the waves trigger biological processes rather than tissue trauma. LiSWT has been shown to stimulate angiogenesis, improve circulation, and modulate inflammatory responses. Because the treatment is well tolerated, it is performed in brief outpatient sessions without anesthesia.
High-intensity shockwave therapy operates above 0.2 mJ/mm². The energy is concentrated at a focal point to create mechanical force, often strong enough to fragment calcifications or induce controlled microtrauma that jump-starts the healing process. This intensity makes treatment uncomfortable, frequently requiring anesthesia, and sessions are typically limited to one or two.
How Do Low- and High-Intensity Shockwaves Differ?
Although both modalities employ shock waves, their delivery and patient experience differ substantially. Below, we compare LiSWT and HiSWT across several aspects:
How They Work
Low-intensity shockwave therapy disperses lower-energy parallel waves across a wide area of tissue. This diffusion allows the energy to reach both superficial and deeper layers while avoiding damage. High-intensity shockwave therapy, in contrast, relies on lenses or reflectors that converge the energy into a small focal zone, delivering very high pressure to one precise spot.
Mechanism of Action
LiSWT primarily activates biological repair mechanisms. Research shows increased vascular endothelial growth factor (VEGF), endothelial nitric oxide synthase (eNOS), and improved microcirculation. Studies also demonstrate immune modulation, shifting macrophages toward pro-healing phenotypes (Guo et al. 2022; Holsapple et al. 2021).
HiSWT acts mainly through mechanical disruption. It can fragment calcifications or hard tissue, producing immediate structural changes. Higher doses are correlated with matrix disruption and cell loss, which explains the frequent need for anesthesia (Poenaru et al. 2022).
Patient Sensation and Side Effects
Patients typically describe LiSWT as a light tapping or pressure sensation. No anesthesia is required, and side effects are minimal, such as temporary redness or soreness. HiSWT is often painful because of the strong focal pressure. Sedation or anesthesia is commonly required, and transient bruising or swelling may occur after treatment.
Number of Sessions Required
LiSWT protocols generally involve three to six weekly sessions, with benefits accumulating over time as angiogenesis and remodeling occur. HiSWT can achieve its goal more rapidly, often in one or two sessions, as the intent is to induce structural disruption rather than gradual regeneration.
Indications and Clinical Versatility
LiSWT is suited to chronic, regenerative conditions such as tendinopathies, diabetic ulcers, and erectile dysfunction. HiSWT is more appropriate when physical breakdown is required, such as shattering kidney stones, treating calcified tendon deposits, or managing delayed bone union.
Therapeutic Outcomes of Low vs High Intensity Shockwave Therapy
To know which approach “works best,” it is helpful to review clinical outcome studies for various conditions. Low-intensity and high-intensity shockwave therapies have both been studied in specific contexts. Below, we summarize key research findings for each modality:
Clinical Outcomes of Low-Intensity Shockwave Therapy
LiSWT has shown efficacy in treating conditions such as:
- Erectile Dysfunction: A randomized crossover trial demonstrated that LiSWT significantly improved erectile function, with SHIM scores elevated at both one and six months. Results demonstrated vascular and regenerative effects, supporting its role in vasculogenic ED (Kennady et al., 2023).
- Diabetic Foot Ulcers: In a Phase III RCT, LiSWT plus standard wound care achieved higher ulcer closure rates than sham, with 35.5% healing at 20 weeks. Findings confirm improved perfusion and tissue regeneration in chronic wounds (Snyder et al., 2018).
- Achilles Tendinopathy: A randomized clinical trial in non-insertional Achilles tendinopathy reported significant pain reduction and functional gains after low intensity shockwave therapy compared with ultrasound therapy. Outcomes support a regenerative effect, with improved gait measures at follow-up (Stania et al., 2024).
- Peyronie’s Disease: LiSWT has supportive evidence for pain relief in Peyronie’s disease. A 2024 systematic review and meta-analysis of controlled trials reported higher rates of plaque reduction and pain improvement, with mixed effects on curvature and sexual function (Li et al., 2024).
Clinical Outcomes of High-Intensity Shockwave Therapy
HiSWT has been used to treat conditions such as:
- Calcific Tendinitis: A randomized trial of 42 patients with calcified rotator cuff tendinopathy reported that high-energy ESWT significantly improved pain and function and reduced deposit size versus routine physiotherapy at short-term follow-up (Ahmad et al., 2022).
- Hip Osteoarthritis: A randomized trial compared HiSWT, radial ESWT, and sham therapy for hip osteoarthritis. Both shockwave groups showed improvements in pain and WOMAC scores, but the focused high-intensity group demonstrated the greatest functional gains. This supports HiSWT as an effective option for symptomatic relief in degenerative hip disease (Şah, 2023).
- Kidney Stones: A 2023 prospective study of distal ureteral stones found that early second-session focused high-energy SWL achieved effectiveness similar to ureteroscopy, with fewer complications and lower cost (Gong et al., 2023).
- Nonunion Fractures: A 2021 retrospective study of high-energy focused ESWT demonstrated strong healing results in humeral delayed unions and nonunions, suggesting a viable alternative to revision surgery (Dahm et al., 2022).
Summary Comparison Table: Low vs High Intensity Shockwave Therapy
| Aspect | Low-Intensity (LiSWT) | High-Intensity (HiSWT) |
| Energy Level | < 0.2 mJ/mm² (low energy) | > 0.2 mJ/mm² (high energy) |
| Effect Type | Biological repair stimulation | Mechanical disruption |
| Sessions | 3–6+ sessions (cumulative) | 1–3 sessions (often single) |
| Tolerance | Comfortable, no anesthesia | Painful; anesthesia is often needed |
| Side Effects | Minimal to none | Bruising and soreness are common |
| Best Uses | ED, wounds, tendinopathies, fasciitis (soft tissue regeneration) | Stones, calcifications, nonunion fractures (hard tissue issues) |
Which Is Best, Low or High Intensity Shockwave Therapy?
Each approach has a defined role. HiSWT is best reserved for structural problems that require mechanical disruption. LiSWT is more adaptable, with a broader range of regenerative applications that fit easily into outpatient practice. For most chronic conditions, its comfort, safety, and biological stimulation make it the more versatile option.
SoftWave Therapy builds on these principles. Using a patented, broad-focused parabolic reflector, SoftWave distributes low-intensity energy across a treatment zone that is both wide and deep, covering up to 7 cm by 12 cm of tissue simultaneously, reaching both superficial and deep structures. This design stimulates angiogenesis, modulates inflammation, and promotes tissue repair without inducing microtrauma, while maintaining high patient comfort. SoftWave is FDA-cleared for multiple indications and is widely used in various medical specialties, including orthopedics, sports medicine, physical therapy, urology, and podiatry.
Learn more about the Best Shockwave Therapy Machine for Providers.
Transform Treatment Outcomes Through SoftWave Therapy
Both modalities have a place in medicine, but low intensity shockwave therapy stands out for its versatility, patient comfort, and regenerative potential. SoftWave Therapy represents the next step in this field, offering a patented design that treats both superficial and deep tissues without causing microtrauma. Its mechanism supports repair through improved circulation and regenerative signaling, providing durable outcomes while remaining comfortable for patients.
What sets SoftWave apart is how seamlessly it integrates into clinical practice. Treatments take only minutes and require no anesthesia, making them efficient for high-volume clinics. With regulatory clearances and adoption across various fields, SoftWave provides physicians with an evidence-based solution to expand treatment options and enhance patient outcomes.
Become a SoftWave Provider today and bring evidence-based innovation into your Practice.