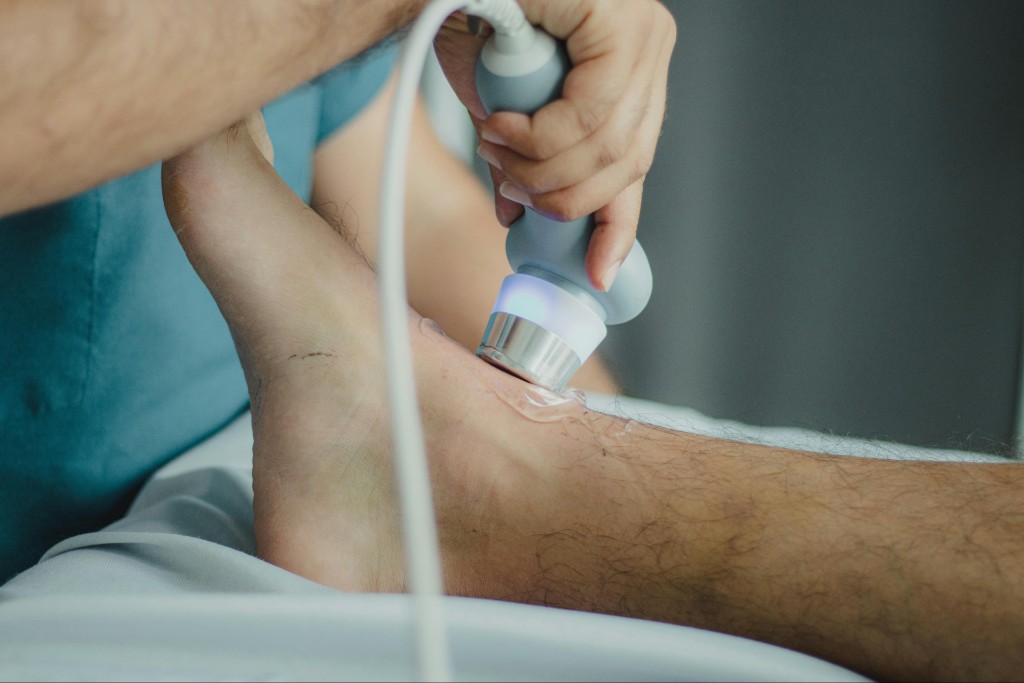
Choosing between shockwave therapy vs ultrasound is a common decision point for clinicians working across orthopedics, sports medicine, urology, and wound care. Both modalities are non-invasive and widely used, yet they operate through very different mechanisms and lead to distinct clinical outcomes. Recognizing how these differences translate into patient indications and long-term results helps providers select the approach that best supports their clinical objectives.
Key Differences Between Shockwave Therapy and Therapeutic Ultrasound
Both shockwave therapy and therapeutic ultrasound deliver energy into tissues, but they do so in fundamentally different ways. ESWT devices generate pulses that propagate as shockwaves through the body, whereas ultrasound machines produce high-frequency sound vibrations (typically 1–3 MHz) that travel as ultrasonic waves. Below, we explore the main differences between these two treatment modalities in terms of how they work, how deeply they act, and the responses they trigger in the body.
Mechanism of Action and Energy Delivery
Shockwave therapy delivers high-pressure acoustic pulses that create mechanical stress in tissues, stimulating cellular repair and biological healing. Therapeutic ultrasound instead uses continuous or pulsed high-frequency sound waves that primarily generate deep heating and mild mechanical vibration. Shockwaves are mechanotransductive in nature, while ultrasound mainly achieves thermal and circulatory effects.
Treatment Depth and Energy Penetration
Shockwaves can penetrate 5–12 cm, depending on device type, reaching both superficial and deep structures, including tendons and bone interfaces. Ultrasound is effective within a tissue depth of 2–5 cm, with higher frequencies targeting more superficial tissues. Because ultrasound energy attenuates quickly, it is best suited for moderately deep or surface-level structures.
Biological Response and Healing Effects
Shockwaves initiate regenerative cascades by promoting angiogenesis, releasing growth factors, and modulating chronic inflammation. These effects contribute to durable improvements in tendon, bone, and wound healing. Ultrasound primarily improves local circulation through thermal effects, reduces stiffness, and relaxes soft tissues. Non-thermal ultrasound may provide mild collagen remodeling, though its impact is less regenerative compared to shockwaves.
Sessions Required
Shockwave therapy is typically administered once a week for 3–6 sessions, as its biological effects unfold gradually. Ultrasound treatments are shorter but often require a higher frequency, typically 2–3 times weekly over 4–6 weeks. Shockwave therapy, therefore, achieves outcomes in fewer total visits, while ultrasound relies on cumulative applications for benefit.
Side Effects and Safety Profile
Shockwave therapy is well-tolerated, with patients sometimes experiencing mild soreness or redness that typically subsides within hours. Ultrasound therapy is also safe, producing a gentle warming effect during application. Both modalities carry very low risk when performed correctly, though improper ultrasound technique can occasionally lead to localized overheating.
Clinical Uses and Medical Indications
Shockwave therapy excels in treating chronic or hard-to-heal musculoskeletal conditions and promoting regeneration. It is commonly used for conditions such as plantar fasciitis, Achilles tendinopathy, lateral epicondylitis, calcific tendon deposits, non-union fractures, and urologic conditions. Ultrasound is more often used for acute or subacute soft-tissue injuries, muscle strains, bursitis, tendonitis, myofascial pain, and adjunct wound care. It is also used in phonophoresis to enhance the absorption of medication.
Patient Comfort and Treatment Experience
Shockwave sessions last 5–15 minutes and are felt as rapid tapping sensations that patients tolerate well. Ultrasound treatments are painless, experienced as a gentle warmth with steady movement of the probe over the skin. Post-treatment, shockwave patients may notice temporary soreness, while ultrasound doesn’t produce after-effects.
Treatment Outcomes and Efficacy of Shockwave Therapy and Therapeutic Ultrasound
Clinical research has investigated the effectiveness of both shockwave therapy and therapeutic ultrasound in treating various conditions. Below, we highlight recent evidence on outcomes for common indications, giving a sense of the efficacy of each modality.
Treatment Outcomes and Efficacy of Shockwave Therapy
- Chronic Plantar Fasciopathy: In a randomized trial, shockwave therapy resulted in significant pain relief and functional improvement in chronic plantar fasciitis, with the benefits sustained for two years, compared to a placebo (Ibrahim et al., 2017). This long-term effect suggests shockwaves stimulate true healing rather than temporary relief.
- Lateral Epicondylitis: A 2024 double-blind RCT found shockwave therapy reduced pain and disability scores, achieving near-normal elbow function by week 7 (Perveen et al., 2024). These outcomes highlight ESWT’s superiority in chronic tendon pathology.
- Achilles Tendinopathy: In a randomized trial of 39 patients, shockwave therapy showed greater improvement in pain and function for chronic Achilles tendinopathy after 6 weeks (Stania et al., 2024). Findings support ESWT as a first-line option in stubborn tendon disorders.
- Diabetic Foot Ulcers: A phase III multicenter trial found 35.5% of diabetic foot ulcers healed with focused shockwave therapy by 20 weeks, compared to 24.4% in controls (Snyder et al., 2018). This shows shockwaves enhance perfusion and growth factor release, improving wound closure rates.
Treatment Outcomes and Efficacy of Therapeutic Ultrasound
- Knee Osteoarthritis: A meta-analysis of five RCTs showed low-intensity pulsed ultrasound significantly reduced pain and improved function in knee osteoarthritis compared to controls (Zhou et al., 2018). Findings support the use of ultrasound as a safe adjunct for symptom relief.
- Myofascial Pain Syndrome: In a placebo-controlled trial, therapeutic ultrasound applied to trapezius trigger points reduced pain and improved pressure thresholds compared to sham treatment (Yildirim et al., 2018). This validates ultrasound as effective for managing myofascial pain.
- Rotator Cuff Tendinopathy: A RCT reported that therapeutic ultrasound significantly reduced pain and improved shoulder function in patients with chronic rotator cuff tendinopathy (Diyarbakır et al., 2025). These findings reinforce the use of ultrasound as an effective option for managing persistent shoulder conditions.
- Pressure Ulcers: A controlled trial demonstrated that therapeutic ultrasound, when added to standard care, reduced pressure ulcer size by 63% over 12 weeks, indicating clear healing benefits (Karslı et al., 2017). These results highlight ultrasound as a supportive modality for managing chronic wounds.
Comparative Table: Shockwave Therapy vs Therapeutic Ultrasound
| Aspect | Shockwave Therapy (ESWT) | Therapeutic Ultrasound |
| Mechanism | High-pressure acoustic pulses; mechanical stimulation and tissue regeneration | High-frequency sound waves; thermal and circulatory effects |
| Depth | Reaches 5–12 cm, effective for deep and superficial tissues | Effective 2–5 cm, best for moderate or superficial tissues |
| Biological Effects | Stimulates angiogenesis, growth factors, stem cells, and reduces chronic inflammation | Increases circulation, decreases stiffness, relaxes muscles |
| Sessions | Fewer, spaced sessions (3–6 total) with lasting outcomes | More frequent sessions (8–15 total) are needed for effect |
| Safety | Mild, short-lived soreness possible; safe overall | Comfortable, painless; rare overheating risk |
| Indications | Chronic tendinopathies, plantar fasciitis, calcific deposits, bone healing, wounds, urology | Acute/subacute injuries, sprains, bursitis, myofascial pain, wound adjuncts |
Benefits of Shockwave Therapy Vs Therapeutic Ultrasound
Therapeutic ultrasound is appreciated for its comfort, safety, and ease of use in rehabilitation. It supports circulation, reduces stiffness, and can be useful in acute or subacute injuries. While versatile and widely accessible, its effects are often more supportive than regenerative, making it a helpful adjunct rather than a stand-alone solution for long-term outcomes.
Shockwave therapy, in contrast, actively stimulates tissue repair through angiogenesis, growth factor release, and modulation of inflammation. This regenerative capacity makes it especially effective in chronic or resistant conditions, often requiring fewer sessions with results that last well beyond treatment. Modern innovations such as SoftWave Therapy have further advanced this field, offering broad-focused energy delivery that enhances outcomes while maintaining patient comfort.
Want to learn more about the benefits of shockwave therapy? Explore the Best Shockwave Therapy Machine for Providers.
Improve Patient Outcomes with SoftWave Therapy
While both modalities have their place, shockwave therapy stands out for its ability to stimulate regenerative healing and deliver lasting outcomes. Ultrasound remains a helpful option in acute care and as an adjunct, offering comfort and supportive benefits. Taken together, these differences enable providers to choose the approach that best suits patient needs, with shockwave therapy often emerging as the more comprehensive solution.
SoftWave Therapy represents the latest advancement in shockwave technology, delivering patented and FDA-cleared broad-focused waves that reach both superficial and deep tissues without causing microtrauma. Supported by clinical research, it has been integrated across orthopedics, sports medicine, physical therapy, urology, and podiatry to improve outcomes while fitting seamlessly into clinical workflows.
Become a SoftWave Provider today to expand your treatment capabilities and offer patients a proven, regenerative solution.