Regenerative treatments in sports and orthopedic medicine continue to reshape how clinicians approach musculoskeletal healing. These therapies focus on stimulating biologic processes such as angiogenesis and cellular repair to restore tissue function without invasive procedures. Orthopedic and sports medicine specialists are integrating these approaches to meet growing clinical demands for non-surgical solutions that support durable recovery. As protocols evolve, regenerative options are becoming more prominent in the management of complex soft tissue and joint conditions across outpatient settings.
The Role of Regenerative Treatments in Sports and Orthopedic Medicine Practice
Musculoskeletal care is shifting toward strategies that modulate healing biology at the tissue level. Regenerative approaches target angiogenic signaling, controlled inflammatory pathways, and extracellular matrix remodeling to promote structural restoration and sustained function. Evidence syntheses describe expanding clinical use of biologic agents such as platelet-rich plasma and stem cell therapy, which enhance intrinsic repair mechanisms in orthopedic indications and show measurable improvements in pain and function when applied within evidence-based protocols (Mavrogenis et al., 2023).
In parallel, biophysics-based interventions such as shockwave therapy and low-level laser therapy are being incorporated into regenerative rehabilitation frameworks, where physical energy stimuli activate cellular pathways that contribute to tissue recovery and functional restoration (De Sire et al., 2023). Together, these lines of evidence illustrate a move toward protocols that emphasize biologic repair, measurable function, and reduced reliance on purely symptomatic care.
Exploring Effective Regenerative Treatments in Orthopedic and Sports Medicine
Regenerative treatments in sports and orthopedic medicine are increasingly recognized for their ability to promote biologic healing by controlling the activation of cellular repair pathways. These modalities rely on mechanical, biochemical, or biophysical mechanisms to restore tissue structure and function, providing clinicians with evidence-based, non-surgical options for musculoskeletal care.
Shockwave Therapy
Extracorporeal shockwave therapy (ESWT) is a non-invasive modality that delivers acoustic waves into targeted tissue to stimulate biologic repair. The treatment promotes angiogenesis, modulates inflammation, and activates cellular signaling pathways that support tissue remodeling. It is widely used for both chronic and acute musculoskeletal conditions due to its reproducible outcomes and minimal patient discomfort. Clinical studies using SoftWave devices (one of the most advanced ESWT devices) have demonstrated consistent improvements in pain and function across tendinopathies and chronic pain presentations, with high levels of patient satisfaction following short treatment protocols (Fansa et al., 2021). Through its ability to enhance vascular regeneration and improve local metabolism, shockwave therapy has become a core modality in regenerative orthopedic and sports medicine care.
SoftWave Therapy in Regenerative Orthopedic and Sports Care
SoftWave Therapy represents an advancement in shockwave technology, designed for clinicians seeking to achieve consistent regenerative outcomes through evidence-based treatment. Its patented, broad-focused applicator distributes shock waves evenly across both superficial and deep tissues, stimulating angiogenesis, activating connective tissue, and modulating inflammatory pathways without causing microtrauma. Supported by FDA clearances, SoftWave Therapy offers short, well-tolerated sessions that integrate efficiently into orthopedic and sports medicine protocols, providing measurable improvements in tissue regeneration and patient function.
Learn how clinics are improving patient outcomes with the best shockwave therapy machine for providers.
Platelet-Rich Plasma (PRP)
PRP therapy uses concentrated autologous platelets to release growth factors that promote fibroblast activity, collagen production, and angiogenesis. Meta-analytic evidence across chronic musculoskeletal conditions, including osteoarthritis and tendinopathies, demonstrates measurable improvements in pain and function when preparation and administration parameters are standardized (Laudy et al., 2021). Outcomes are influenced by platelet concentration and activation methods, which affect biologic response and treatment consistency. PRP is frequently incorporated into multimodal rehabilitation programs, where its ability to modulate inflammation and support tissue repair complements other regenerative approaches.
Stem Cell Therapy
Stem cell therapy involves the use of mesenchymal stem cells that can differentiate into musculoskeletal tissues and release bioactive molecules to support regeneration. Meta-analyses report measurable improvements in pain and function across degenerative musculoskeletal disorders, along with favorable safety profiles and continued research refining optimal cell sources and delivery protocols (Cao et al., 2025). Stem cell applications are typically performed in specialized facilities and are often included as part of comprehensive regenerative strategies in orthopedic medicine.
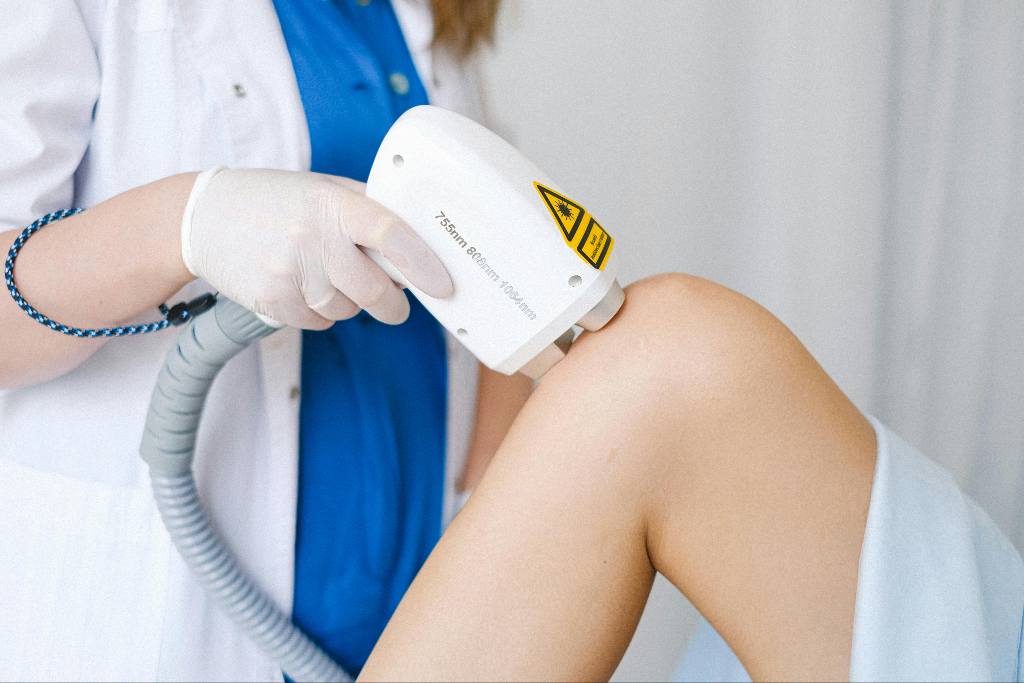
Low-Level Laser Therapy (LLLT)
Low-Level Laser Therapy, or photobiomodulation, uses low-intensity light energy to activate mitochondrial function and enhance cellular metabolism. This process promotes anti-inflammatory effects and tissue regeneration through improved microcirculation and collagen remodeling. Controlled trials have reported reductions in pain and improved function across chronic musculoskeletal conditions when appropriate wavelength and dosage parameters are applied (Dima et al., 2017). The therapy is used as part of individualized rehabilitation programs that support tissue recovery and functional improvement.
Pulsed Electromagnetic Field (PEMF) Therapy
PEMF therapy applies low-frequency electromagnetic fields that modulate ion transport and cellular activity involved in tissue repair. Electromagnetic signals enhance microcirculation, improve oxygen exchange, and stimulate nitric oxide pathways that support healing. In chronic musculoskeletal pain conditions, including knee and hand osteoarthritis, meta-analytic evidence shows improvements in pain and function with strong safety outcomes (Wu et al., 2018). PEMF is commonly used as a complementary modality in multidisciplinary orthopedic and rehabilitation programs to support musculoskeletal health and recovery.
Comparative Overview of Regenerative Modalities in Orthopedic and Sports Medicine
Clinicians evaluating regenerative technologies often compare treatment mechanisms, biologic scope, and ease of integration into practice. Each modality supports healing through distinct cellular pathways, though differences in treatment area, precision, and workflow can affect outcomes. The table below outlines core clinical characteristics relevant to orthopedic and sports medicine applications.
| Modality | Mechanism of Action | Clinical Applications | Key Considerations |
|---|---|---|---|
| SoftWave Therapy | Broad-focused shock waves activate angiogenesis, modulate inflammation, and stimulate cellular repair in both superficial and deep tissues without microtrauma. | Musculoskeletal injuries, chronic pain, tendinopathies, and wound healing. | FDA-cleared for connective tissue activation. Provides consistent, evidence-based outcomes across a wide range of treatment areas in short, well-tolerated sessions. |
| Platelet-Rich Plasma (PRP) | Concentrated platelets release growth factors that support tissue remodeling. | Tendinopathies, mild joint degeneration, soft tissue injuries. | Outcomes vary with platelet concentration and activation methods. |
| Stem Cell Therapy | Mesenchymal stem cells release bioactive mediators that aid repair. | Cartilage and soft tissue degeneration, joint disease. | Specialized procedure with an ongoing study on standardization. |
| Low-Level Laser Therapy (LLLT) | Low-intensity light energy enhances mitochondrial function and microcirculation. | Chronic pain, inflammation, soft tissue injuries. | Non-invasive and well-tolerated. Effects depend on wavelength and frequency. |
| Pulsed Electromagnetic Field (PEMF) Therapy | Electromagnetic fields modulate ion exchange and nitric oxide signaling to support healing. | Joint and soft tissue disorders, rehabilitation. | Safe, non-invasive, and commonly used as an adjunct. |
Among the most utilized regenerative modalities in orthopedic and sports medicine, SoftWave Therapy devices demonstrate a distinctive combination of biologic precision and clinical efficiency. Its patented parabolic reflector produces a treatment field measuring approximately 12 cm by 7 cm, allowing uniform energy distribution across deep and superficial tissues in a single application. This broad therapeutic zone enables effective coverage of complex musculoskeletal structures while maintaining patient comfort and procedural consistency. For clinicians, this scalability supports streamlined workflows and reliable outcomes across a range of regenerative indications.
Transform Your Clinical Approach to Regenerative Care with SoftWave Therapy
Regenerative treatments are reshaping orthopedic and sports medicine as clinicians adopt biologic modalities that stimulate natural healing while minimizing intervention. These advancements reflect a broader shift toward biologic restoration and functional recovery supported by measurable clinical outcomes. SoftWave Therapy embodies this progress through its evidence-based approach to tissue regeneration and its expanding role in musculoskeletal care.
Applied across orthopedics, sports medicine, physical therapy, urology, and podiatry, SoftWave Therapy has become an integral part of modern regenerative practice. Its clinical validation and growing body of research highlight its effectiveness in enhancing patient outcomes while aligning with the operational needs of high-performing medical environments.
Become a SoftWave Provider today and join the growing network of clinicians dedicated to regenerative excellence.